Benefits
Open Enrollment
Open Enrollment IS NOW CLOSED
5 Steps to a Successful Open Enrollment

Please review the updates and information regarding this year's Open Enrollment changes, including activities and helpful links for learning about your benefit options.
Open Enrollment begins: Ended
Open Enrollment ends: Ended
Benefits Fair: Ended
 1. Update Contact Information: Ensure that you receive all benefit-related information in a timely manner by updating
your contact information. This requires updating your email in People First.
1. Update Contact Information: Ensure that you receive all benefit-related information in a timely manner by updating
your contact information. This requires updating your email in People First.
Update Contact Information
The State of Florida will be distributing benefit plan information. Please verify that your email and mailing address is correct to ensure that your benefits plan information is delivered.
EMAIL ADDRESS UPDATE
Follow these steps to verify/update your email in People First:
(Click here for instructions with pictures).
- Go to https://peoplefirst.myflorida.com/peoplefirst/index.html
- Sign in with your People First ID and password.
- Click "Contact Information"
Verify your email or update to your correct email address - To edit, click on the "Notification Email" row and click the edit button.
- Update the email address and click "Save"
- Confirmation will pop up
MAILING ADDRESS UPDATE
Please review your contact information in People First and Oracle HR to ensure that
you receive all benefit-related information in a timely manner. Any updates made in
Oracle HR are sent automatically to People First each night.
Instructions to update address in OracleHR.
Using the MyUSF portal, navigate to the "Business Systems" dropdown menu and choose "Oracle HR"

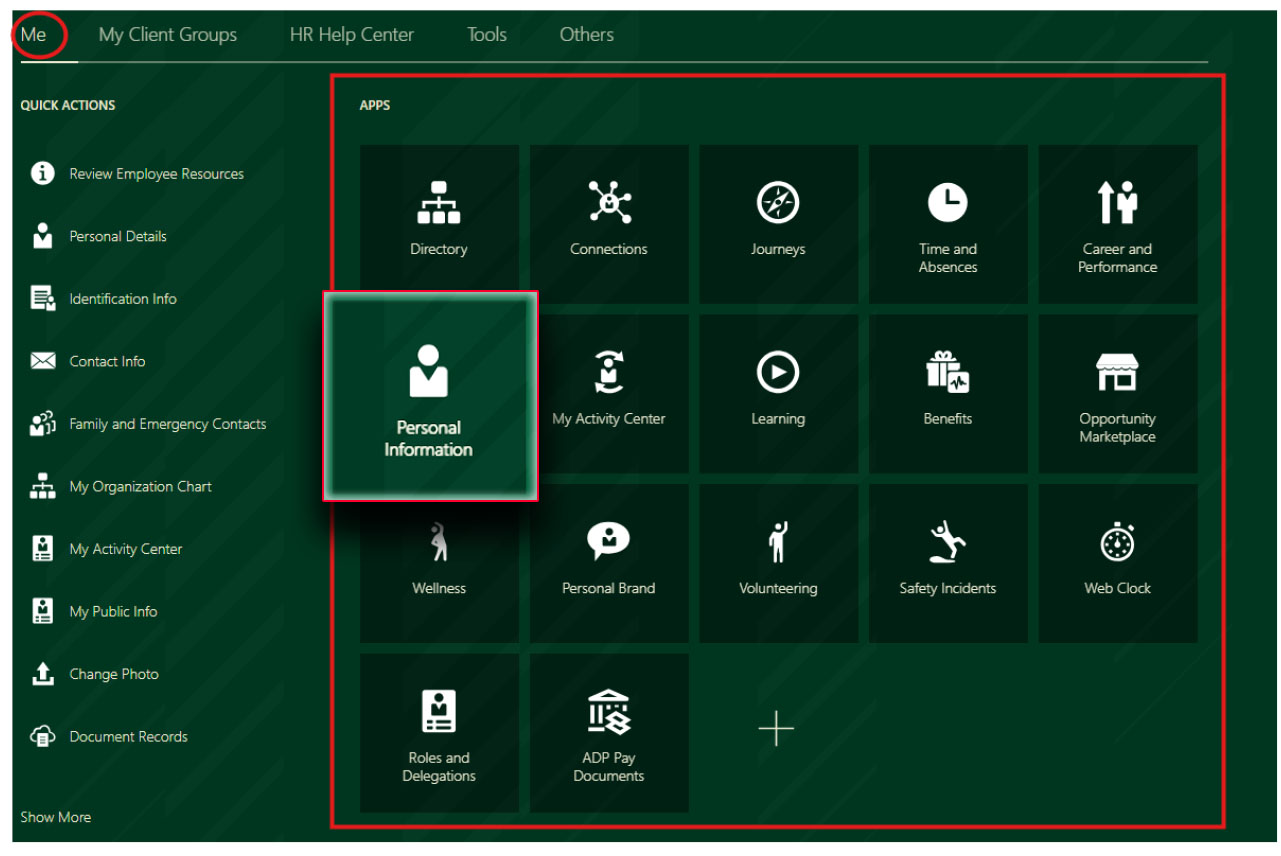
From the "Me" menu, click the "Personal Information" tile.
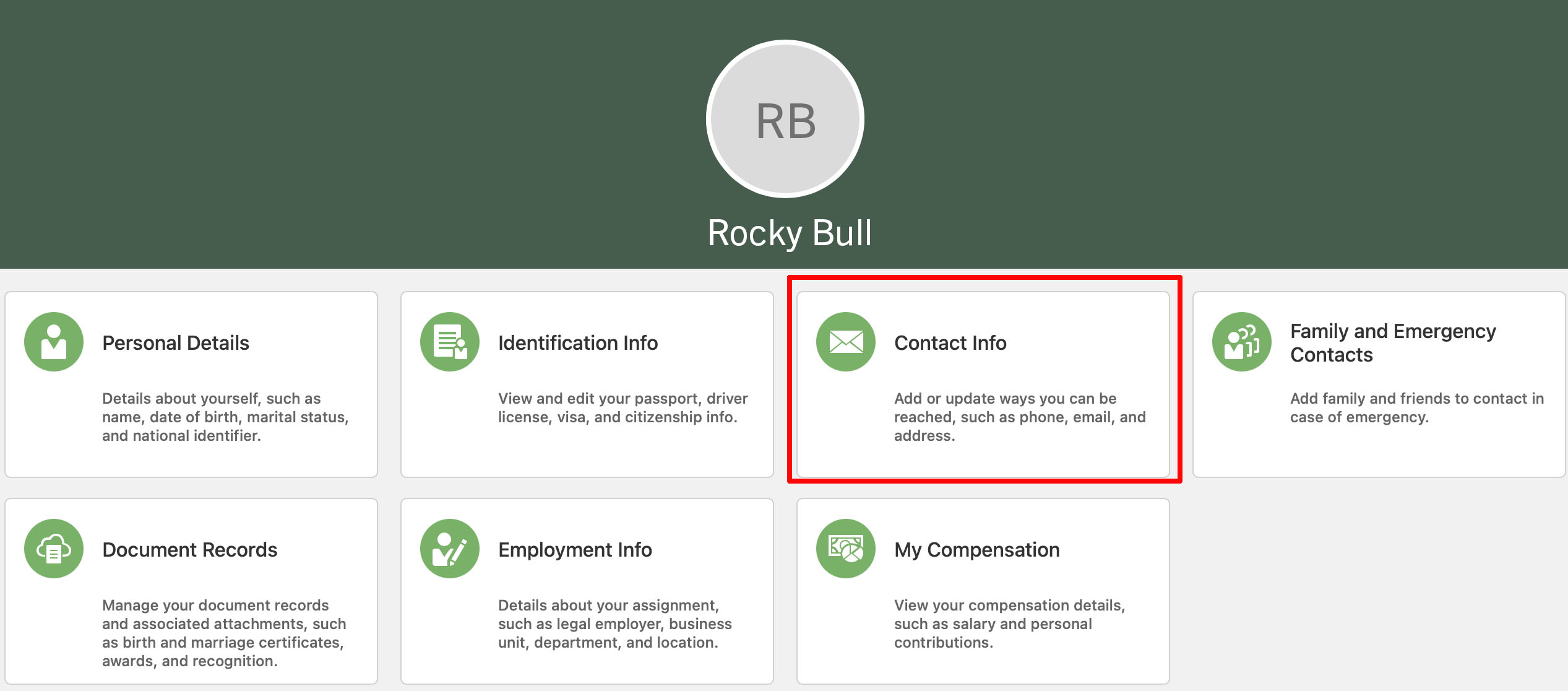
Select the "Contact Information" card. A screen will open, allowing you to edit and save your contact details.
PEOPLE FIRST PASSWORD UPDATE
In addition to the address verification, you are encouraged to update your password
so you will not have to reset it during Open Enrollment. Please note that the following
will be required for password reset online: (1) A notification email set-up OR (2)
a phone number able to receive text messages. If you do not have these reflected
at People First, you will need to contact the People First Service Center and may
experience long wait times due to high call volumes. You can access the People First login screen here to reset your password. Information on how to reset your password can be found on
the People First website’s Frequently Asked Questions.

2. Don't miss out on what's new for the next plan year.
Click here for information on the 2026 plan year benefits.
What's Changing?
NEW LIFE INSURANCE CARRIER - METLIFE
The State of Florida is pleased to announce MetLife as our new Basic and Optional
Term life Insurance provider beginning Jan.1,2026. Plans currently in place will automatically
roll over to MetLife, including beneficiaries.
| Amount | Rate | |
|---|---|---|
| OPS | $25,000 | $3.18 |
| Retiree | $2,500 | $6.38 |
| Retiree | $10,000 | $25.51 |
- Accidental death and dismemberment insurance will no longer be offered under the new plan.
- Optional term life rater have decreased. Plan information will be mailed by MetLife
to members during Open Enrollment.
2026 INSURANCE PREMIUM CHANGES
- Health premium increases for employers and COBRA participants.
- Dental and vision premium increase for most plans.
Members can view the premiums on the MyBenefits.MyFlorida.com
2026 HIGH-DEDUCTIBLE HEALTH PLAN CHANGES
Deductibles have increased for the 2026 plan year
| Single | Family |
|---|---|
| $1,700 | $3,400 |
2026 PREMIUM FOR CIGNA'S HOSPITAL SUPPLEMENTAL PLAN DECREASES
CHLIC Hospital Supplemental Plan (8100, 8110, 8120, 8130, 8140, and 8150) rates have
decreased for the 2026 plan year. If members wish to continue their existing plan(s),
the premiums will automatically change; members do not need to take any action. Members
considering changing plans during open enrollment should look at the 2026 Monthly
Premium sheet.
SAVINGS AND SPENDING ACCOUNTS INCREASES
Annual maximum increases effective Jan. 1, 2026.
| Individual | Family | 55+ | |
|---|---|---|---|
| HSA | $4,400 | $8,750 | $1,000 |
| Single/Married Filing Jointy | Married/Filing Separately | ||
| FSA Dep Care | $7,500 | $3,750 | |
MEDICARE ADVANTAGE PRESCRIPTION DRUG PLANS THAT OFFER PRESCRIPTION DRUG COVERAGE
If you and/or your dependent(s)are enrolled in Medicare Part A and Part B, new MA-PD
plan options are currently in the process of being re-procured and may not be available
for selection during standard open enrollment. As a result, this benefits statement
will show all current MA-PD members as enrolled in the Florida Blue PPO Medicare plan
starting January 1, 2026. You will remain enrolled in your current MA-PD plan through
December 31, 2025.
While a new plan may not be available on January 1st, rest assured that new MA-PD plans will be available for selection during the 2026 plan year. Once the new MA-PD plans and prices are finalized, you will be notified and provided with the opportunity to participate in a special open enrollment to select or make changes to your plan. Additional details, including special open enrollment instructions and timelines, will be sent directly to each eligible member from the Division of State Group Insurance. Please watch for this important information in the future.
 3. The USF Benefits Fair and Wellness Expo was held on October 13, 2025
3. The USF Benefits Fair and Wellness Expo was held on October 13, 2025
See more details about offerings on the Tampa campus
Did you know? The Tampa campus features a year-round Working Bulls Sick Clinic.
Benefits Fairs for the 2026 Plan Year Have Concluded
Sarasota-Manatee Employees
See more details about Sarasota-Manatee Campus offerings
Sarasota-Manatee Health Services
The Sarasota-Manatee campus has an on-site Working Bulls Sick Clinic.
 4. Open Enrollment is your once-a-year opportunity to make any changes you want to your State Group Insurance benefits.
4. Open Enrollment is your once-a-year opportunity to make any changes you want to your State Group Insurance benefits.
Make Enrollment Elections
Open Enrollment is your once-a-year opportunity to make any changes you want to your State Group Insurance benefits. You can change your benefits as many times as you want before the deadline.
Accessing People First (Video 3 minutes) Learn about your options to make your elections and tips for accessing the People First portal including finding your People First log in ID and resetting your password.
Navigating the People First portal (Video 7 minutes) Please use Firefox or Google Chrome and disable pop-ups to view this video: A step-by-step guide to enrolling on the People First portal
Log in to People First to make your choices (changes, additions, and/or drop in coverages) and remember to select the Complete Enrollment button when you are ready to save changes. If you make Open Enrollment changes, look for a mailed confirmation statement in early November. Be sure all changes are correct, any eligible dependents are enrolled in coverage, and any ineligible dependents have been removed.
 5. Premiums are deducted a month in advance so it is important to review your benefits deductions on December 2025 and January 2026 paychecks.
5. Premiums are deducted a month in advance so it is important to review your benefits deductions on December 2025 and January 2026 paychecks.
Review Premium Deductions
Please note that benefits premiums are deducted a month in advance so it is important to review your deductions on December 2025 paychecks for changes and notify us at Benefits@usf.edu with any discrepancies.
Health Savings Account and Flexible Spending Account contributions are deducted during the coverage month. Any changes to these accounts will begin with January 2026 paychecks.
If you have questions about your benefits, please contact the Central HR Benefits team or Regional HR Office.
| Date | Time | Topic | Teams Meeting Link |
|---|---|---|---|
| Check back next year! |